Chicagoland’s premier Head and Neck Surgeons. ENT Surgical Consultants is proud to serve our patients with outstanding, comprehensive, cutting edge, and state-of-the-art diagnostic Head and Neck Care. Please contact us today for a consultation 815-725-1191.
Facial nerve injury is a devastating surgical complication. It can produce severe changes in facial appearance, expose the eye to infection and complications that can compromise vision, and cause drooling and changes in vocal quality.
Patients who have had severe facial nerve injury can have lowered self-image and loss of self-confidence and self-esteem. Many have reported boughts of depression. These issues can affect both patients work life and social interactions.
NIM-Response® 2.0
Nerve Integrity Monitoring System
A new level of sensitivity and convenience in nerve monitoring
Monitoring of the facial nerve continuously evaluates the activity in the monitored facial muscles. Both a graphic signal, which can be seen on a screen, and an sound signal, which can be heard throughout the procedure room, are generated.
The three ways that cancer spreads in the body are:
When cancer cells break away from the primary (original) tumor and travel through the lymph or blood to other places in the body, another (secondary) tumor may form. This process is called metastasis. The secondary (metastatic) tumor is the same type of cancer as the primary tumor. For example, if breast cancer spreads to the bones, the cancer cells in the bones are actually breast cancer cells. The disease is metastatic breast cancer, not bone cancer.
Fine needle aspiration is a technique that allows a biopsy of various bumps and lumps. It allows your otolaryngologist to retrieve enough tissue for microscopic analysis and thus make an accurate diagnosis of a number of problems, such as inflammation or even cancer.
A mass or lump sometimes indicates a serious problem, such as a growth or cancer*. While this is not always the case, the presence of a mass may require FNA for diagnosis. Your age, sex and habits, such as smoking and drinking, are also important factors that help diagnosis of a mass. Symptoms of ear pain, increased difficulty swallowing, weight loss or a history of familial thyroid disorder or of previous skin cancer (squamous cell carcinoma) may be important as well.
FNA is generally used for diagnosis in areas such as the neck lymph nodes or for cysts in the neck. The parotid gland (the mumps gland), thyroid gland and other areas inside the mouth or throat can be aspirated as well. Virtually any lump or bump that can be felt (palpated) can be biopsied using the FNA technique.
Your doctor will insert a small needle into the mass. Negative pressure is created in the syringe, and as a result of this pressure difference between the syringe and the mass, cellular material can be drawn into the syringe. The needle is moved in a to-and-fro fashion, obtaining enough material to examine under a microscope and make a diagnosis. The procedure is usually repeated several times to insure adequate sampling of the lump. This procedure is quite accurate and frequently prevents the patient from having an open surgical biopsy, which is more painful and costly.
The procedure generally does not require anesthesia, yet your doctor usually injects a small amount of local anesthetic into the skin. It is slightly more uncomfortable than drawing blood from the arm for laboratory testing. In fact, the needle used for FNA is smaller than that used for drawing blood. Although not painless, any discomfort associated with FNA is usually minimal.
No medical procedure is without risks. Due to the small size of the needle, the chance of spreading a cancer or finding cancer in the needle path is very small. Other complications are rare; the most common is bleeding. If bleeding occurs at all, it is generally seen as a small bruise. Patients who take aspirin, Advil or blood thinners, such as Coumadin, are more at risk to bleed. However, the risk is minimal. Infection is rarely seen.
A tracheostomy is a surgical procedure to create an opening through the neck into the trachea (windpipe). A tube is usually placed through this opening to provide an airway and to remove secretions from the lungs. This tube is called a tracheostomy tube or trach tube.
A tracheostomy may be done if you have:
If the tracheostomy is temporary, the tube will eventually be removed. Healing will occur quickly, leaving a minimal scar.
Occasionally a stricture, or tightening, of the trachea may develop, which may affect breathing.
If the tracheostomy tube is permanent, the hole remains open and may require surgical closure when no longer needed.
Most patients require 1 to 3 days to adapt to breathing through a tracheostomy tube. It will take some time to learn how to communicate with others. Initially, it may be impossible for the patient to talk or make sounds.
After training and practice, most patients can learn to talk with a tracheostomy tube. Patients or family members learn how to take care of the tracheostomy during the hospital stay. Home-care service may also be available.
Normal lifestyles are encouraged and most activities can be resumed. When outside, a loose covering (a scarf or other protection) for the tracheostomy stoma (hole) is recommended. Patients must adhere to other safety precautions regarding exposure to water, aerosols, powder, or food particles as well.
Laryngectomy is surgery to remove the larynx (voice box) in your throat. All or part of the larynx may be removed in a laryngectomy.
Total laryngectomy is major surgery that is done in the hospital. Before surgery you will receive general anesthesia. This will make you unconscious and unable to feel pain.
In a total laryngectomy, first your surgeon will make an incision (cut) in your neck to open up the area. Important parts of this surgery are:
Usually laryngectomy is done to treat cancer of the larynx. It is also done to treat:
You will have many doctor visits and medical tests before you have surgery. Some of these are:
Always tell your doctor or nurse:
During the days before your surgery:
On the day of your surgery:
You will need to stay in the hospital for several days after surgery.
After the procedure, you will be groggy and will not be able to speak. An oxygen mask will be on your stoma. It’s important to keep your head raised, rest a lot, and move your legs from time to time to improve blood flow. Keeping blood moving reduces your risk of getting a blood clot.
You can use warm compresses to reduce pain around your incision. Your nurse will give you pain medicine.
You will receive nutrition through an IV (a tube that goes into a vein) and tube feedings. Tube feedings are given through a tube that goes through your stoma and into your esophagus (swallowing tube).
You may be allowed to swallow food as soon as 2 to 3 days after surgery. But, it is more common to wait 5 to 7 days after your surgery to start eating through your mouth.
Your trachea drain will be removed in 2 to 3 days. You will be taught how to care for your tracheostomy tube and stoma. You will learn how to safely shower or swim. You must be careful not to let water enter through your stoma.
Speech rehabilitation with a speech therapist will help you relearn how to speak.
You will need to avoid heavy lifting or strenuous activity for about 6 weeks. You may slowly resume your normal, light activities.
Follow up with your doctor as often as your doctor says you need to.
Your wounds will take about 2 to 3 weeks to heal. You can expect full recovery in about a month. Many times, removal of the larynx will take out all the cancer or injured material. People learn how to change their lifestyle and live without their voice box.
Oral cancer includes cancers of the mouth and the back of the throat. Oral cancers develop on the tongue, the tissue lining the mouth and gums, under the tongue, at the base of the tongue, and the area of the throat at the back of the mouth.
Oral cancer accounts for roughly three percent of all cancers diagnosed annually in the United States, or about 49,700 new cases each year.
Oral cancer most often occurs in people over the age of 40 and affects more than twice as many men as women. Most oral cancers are related to tobacco use, alcohol use (or both), or infection by the human papilloma virus (HPV).
Tobacco and alcohol use. Tobacco use of any kind, including cigarette smoking and chewing tobacco, puts you at risk for developing oral cancers. Heavy alcohol use also increases the risk. Using both tobacco and alcohol increases the risk even further.
HPV. Infection with the sexually transmitted human papillomavirus (specifically the HPV 16 type) has been linked to oral cancers.
Age. Risk increases with age. Oral cancers most often occur in people over the age of 40.
Sun Exposure. Cancer of the lip can be caused by sun exposure.
If you have any of these symptoms for more than two weeks, see a dentist or a doctor.
Because oral cancer can spread quickly, early detection is important. An oral cancer examination can detect early signs of cancer. The exam is painless and takes only a few minutes. Many dentists will perform the test during your regular dental check-up.
During the exam, your dentist or dental hygienist will check your face, neck, lips, and entire mouth for possible signs of cancer.
When oral cancer is detected early, it is treated with surgery or radiation therapy. Oral cancer that is further along when it is diagnosed may use a combination of treatments.
For example, radiation therapy and chemotherapy are often given at the same time. Another treatment option is targeted therapy, which is a newer type of cancer treatment that uses drugs or other substances to precisely identify and attack cancer cells. The choice of treatment depends on your general health, where in your mouth or throat the cancer began, the size and type of the tumor, and whether the cancer has spread.
You should see an, ear, nose, and throat doctor (otolaryngologist)
Oral cancer and its treatment can cause dental problems. It’s important that your mouth is in good health before cancer treatment begins.
See a dentist for a thorough exam one month, if possible, before starting cancer treatment to give your mouth time to heal after any dental work you might need.
Before, during, and after cancer treatment, ask your health care provider for ways to control pain and other symptoms, and to relieve the side effects of therapy.
Salivary glands are located in the mouth. There are three pairs of large salivary glands. Parotid glands are found in front of and just below each ear. Submandibular glands are below the jaw. Sublingual glands are under the tongue. There are also hundreds of smaller glands. These glands make saliva (spit) and empty it into the mouth through openings called ducts. Saliva makes food moist, which helps chewing and swallowing and the digestion of food. Saliva also keeps the mouth clean and healthy because it contains antibodies that kill germs.
If the salivary glands are damaged or aren’t producing enough saliva it can affect taste, make chewing and swallowing more difficult, and increase the risk for cavities, tooth loss, and infections in the mouth.
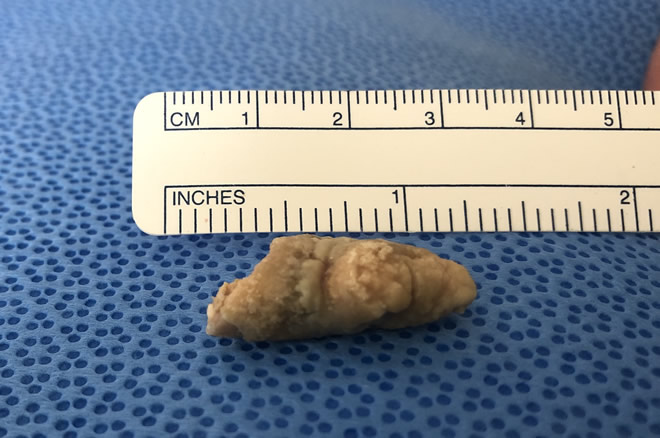 Obstruction: Small stones that form in the gland ducts may obstruct the flow of saliva. The gland may swell and become painful and infected. Small constrictions or twists in the duct system of the large salivary glands can also decrease salivary flow.
Obstruction: Small stones that form in the gland ducts may obstruct the flow of saliva. The gland may swell and become painful and infected. Small constrictions or twists in the duct system of the large salivary glands can also decrease salivary flow.
Infection: When saliva pools behind an obstruction in a duct, the gland can become infected. Infection of the lymph nodes from a sore throat or cold can also cause a secondary infection in the salivary glands.
Tumors: Tumors usually appear as painless enlargements in one of the salivary glands. Malignant (cancerous) tumors often grow quickly, may or may not be painful, and may cause loss of movement in the affected side of the face.
Other Disorders: Diseases such as HIV-AIDS, and autoimmune disorders such as Sjögren's syndrome and rheumatoid arthritis, can make the salivary glands inflamed and painful. Diabetes may also cause enlargement of the salivary glands. Alcoholics may have salivary gland swelling, usually on both sides. Some medications also cause decreased saliva and dry mouth as a side effect.
Problems with salivary glands can cause them to become irritated and swollen. You may have symptoms such as:
A doctor uses your medical history, a physical examination, and laboratory tests to make a diagnosis of a salivary disorder.
If your doctor suspects your pain and inflammation are the result of an obstruction in one of the glands, he or she may order X-rays or ultrasound to identify where the obstruction is and what might be causing it.
If a mass is found in the salivary gland, your doctor will suggest a CT scan or an MRI to get a better look at the problem. Your doctor might also use a fine needle aspiration biopsy to explore further. A lip biopsy of minor salivary glands may be needed to identify certain autoimmune diseases, such as Sjögren’s syndrome.
Salivary disorders are treated according to what is causing them, using medical or surgical treatments. If the salivary disorder is caused by systemic disease (diseases that involve the whole body) then that problem is treated first. This may require a visit to an ENT specialist. If the problem is due to salivary gland obstruction, your doctor might use a probe and dilate the duct to remove the obstructive stone.
If a tumor has developed within the salivary gland, your doctor may recommend its removal. You may be referred to an otolaryngologist (commonly known as an ear, nose, and throat doctor) who performs surgery. Most tumors in the parotid gland area are benign (noncancerous). If a tumor is cancerous, it will be surgically removed and the area treated with radiation therapy afterwards.
Radiation therapy often causes dry mouth, which can increase your risk for cavities and mouth infections. Here are some tips to keep your mouth moist: